John Mwazighe Mnjalla, BScN' 07
When you first meet John
Mwazighe Mnjalla, BScN ’07, he comes across as an unassuming, soft-
spoken and modest man – yet, he is a leader. Since taking over the reins
of a poorly run medical clinic in 2005, Mnjalla has overhauled the
quality of primary healthcare services available for local residents in
the small rural town of Mariakani, 36 kilometres northwest of Mombasa,
Kenya. Today, the Mariakani Community Healthcare Services has earned a
solid reputation for its work in providing basic and preventive
healthcare, and especially in implementing the national HIV programme’s
recommendations.
Why did you feel the need to set up the Mariakani Community Healthcare Services here?
When
I joined the military in 1994,I first worked in Nairobi. Later, I got
posted to Mariakani. While working here, I came across a local clinic
that was being run in an unprofessional manner, with nonmedical staff
actually attending to patients. Most of the patients were ignorant of
this fact, which was further compounded by the unavailability of
essential drugs and medical supplies. In 2003, when the previous owner
vacated the medical clinic, I decided to step in and fill the gap. It
was a huge challenge, as I would attend the clinic after my official
working hours, and work till 11 pm. This was the beginning of the
Mariakani Community Healthcare Services, a local facility aimed at
providing primary healthcare services to the local population in the
area. It complements the government’s facility in the region, which is
overstretched in terms of resources coupled with other challenges such
as accessibility as it is too far away for many people.
How has this public-private partnership helped improve healthcare in the region?
A
public-private partnership is crucial and critical as it directly
benefits the local population. Through such partnerships, there is a
medical referral system for patients. For example, those with severe
hypertension, uncontrolled bleeding after childbirth, road traffic
accidents and those requiring antenatal services can be referred to the
local government healthcare institute, the Mariakani District Hospital.
This has contributed to reducing mortality in this particular region.
How has the Adherence Counselling Centre progressed?
We
opened this centre about seven months ago. It serves those who are
infected or affected by HIV and face stigma and discrimination. Some of
the ways we are impacting lives is by providing employment at the Centre
to those who are living with HIV. We have established provider-
initiated testing and counselling, where every patient can be easily
tested or, at the very least, we ensure that we have a discussion on HIV
and related lifestyle aspects with every patient who comes to us.
Additionally, we have also developed a good rapport with government
institutions and government chemists in Mariakani.
How do you think your AKU education helped you in all that you have achieved so far?
AKU
taught me critical thinking skills. I have a passion to ignite change
in my community and AKU helped me link my education and skills with
service to the community.
What about your work for the Kenyan army’s HIV programme?
I
have been in the Kenya Defence Forces (KDF) for over 14 years and have
been coordinating the KDF HIV Programme for the last three. The
programme focuses on prevention, care and treatment of HIV. It is a
programme anchored by the Ministry of Health in partnership with the
Walter Reed Army Institute of Research.
As a coordinator, I have
been able to influence policy in the KDF HIV programme, especially in
training in different programme areas. I strongly advocated for
localised institutional/barrack based training as opposed to the
external training model previously used, which was very expensive as
participants would have to be accommodated in a hotel. My advocacy for
such training enabled the institution to save funds, which went toward
training more health workers and therefore enhancing the quality of
care. Under this strategy we have managed to train over 400 healthcare
workers across the country in areas such as the prevention of
mother-to-child transmission of HIV and provider-initiated testing and
counselling. As a result, we are seeing an upsurge in HIV testing and
counselling uptake in the KDF.
What is your vision for the future of nursing in East Africa?
Nursing
in East Africa is changing, and the Bachelor of Science in Nursing
degree is making a real difference. AKU has contributed immensely in
making a positive change. AKU alumni are at the forefront, having made
significant contributions to healthcare policy and serving as
influencers in their areas of work like the above mentioned training
strategy for the barracks based training that I developed and
implemented.
Delivering Care at the Primary Level
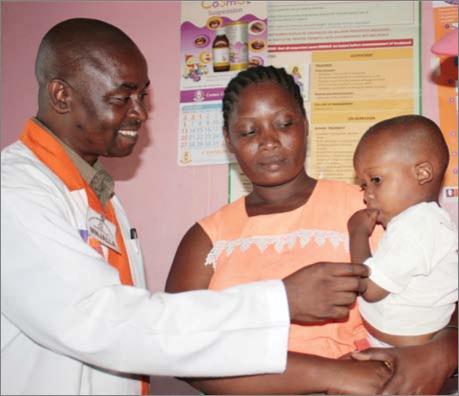
During
the interview with John Mwazighe Mnjalla, a couple arrived at the
clinic with their two-year-old son for a follow-up visit. Their young
child had recently been attacked by a swarm of bees and had been treated
by John. “I had left my son in my neighbour’s care, and when I heard
his screams I rushed over,” the mother narrated. The boy was covered
with bees and the mother and the neighbours desperately tried to brush
them off. However, by the time the father arrived, the child was
beginning to lose consciousness, and so they immediately rushed him to
John’s clinic.
“When I saw the boy, I knew we had to act quickly
as he had become limp and we were in danger of losing him, possibly in a
matter of minutes,” said John. He immediately administered the
treatment and, luckily, the boy began to respond. “The intervention
saved his life,” recalls the boy’s mother. “Were it not for the quick
action taken at the Mariakani Clinic and the diligence and expertise of
the team, I would not want to imagine what would have happened,” she
concluded with a grateful smile.

